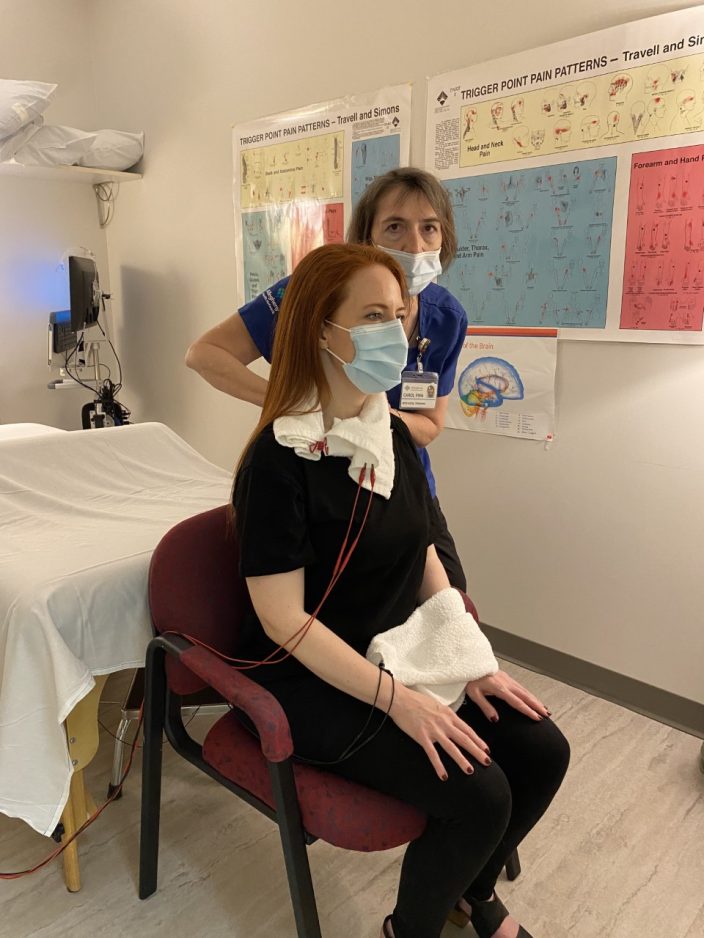
Using trigger points and microcurrents to help patients heal
When Sara Shissler suffered a traumatic brain injury (TMI) in a car accident in 2015, she was looking for help. The Pittsburgh resident was also left with chronic migraines plus neck and shoulder pain. Shissler turned to myofascial trigger point therapist Carol Finn for treatment.
“The trigger point therapy targets the specific areas where the muscles are tight,” Shissler says. “She manually applies pressure to the trigger points to get them to release. It is hard to describe how it feels.”
Myofascial therapy is a non-pharmaceutical, non-invasive form of pain relief that has been around since the 1940s. Also known as trigger point therapy, it focuses on stretching and loosening painful knots in the fascia and muscles and is beneficial in treating headaches, back pain, neck pain and more.
Shissler’s sessions with Finn also include Frequency Specific Microcurrent (FSM) therapy. “The microcurrent can’t be felt itself, but the treatments are extremely relaxing in general, and it also helps muscle tension to release,” says Shissler. “Sometimes it actually puts me to sleep.”
FSM is showing promise in effectively treating patients with TMI by delivering a mild electrical current to affected body parts and alleviating pain by softening the biologic tissue on a cellular level. For these patients, the results can be life-changing. FSM is now being used around the world and in top hospitals such as Cleveland Clinic, Mayo Clinic and Walter Reed Hospital. Finn uses FSM in her practice through Allegheny Health Network at Choice Care Physicians in Pittsburgh.
Finn brings expertise as a licensed massage therapist and certified brain injury specialist to her practice but also knows the effects of traumatic brain injury firsthand.
“I have had several brain injuries,” Finn explains. “I have epilepsy, and these seizures have caused me to fall hard. Several times this has happened in the shower, thus hitting my head on a hard surface.” Looking for ways to help her own recovery, Finn says she treated herself with FSM and believes it has helped. “After some of my brain injuries I have felt like my memory was very shaky,” says Finn. “In the morning I had to stop and think, ‘What do I do next?’ The tremors in hands were bad, causing them to fly off the keyboard when I was typing. Some depression. The FSM helped my brain to heal.”
Finn says her own background has helped her understand patients with TMI better and improves her quality of care for them.
“I don’t know what I would be like if I didn’t have the FSM to treat myself after my injuries,” says Finn. “Because of my own background, I have a sympathy for treating those people with brain injuries. When you break a bone, you break a bone. When you have a head injury, it is you that is broken. I understand the shaky memory, light and smell sensitivity, and so many other things that can be problematic. I may not be able to make everything 100%, but FSM is often able to improve or lessen some of the issues.”
Like Sara Shissler, patients with TMI often also often have neck and shoulder pain. That’s where the myofascial trigger point therapy (MTPT) and FSM together can often help reduce pain. “It focuses on loosening the knots (trigger points) in the muscles and the fascia that are causing pain, discomfort and stiffness,” Finn said. “We find the trigger points, apply pressure that breaks the trigger points up and then do gentle movement.”
Most insurance plans will cover the treatments, so check with your doctor and insurance provider to determine coverage and whether you would be responsible for any co-pays.
Shissler says she has received pain relief and results from her treatments.
“So far I have had excellent results,” says Shissler. “There is less muscle tension and pain in the neck shoulders and head. The migraines are less frequent and less severe.” She’s also felt improvement in her left shoulder, which has given her constant pain since the accident.
“I am pretty much able to move it normally now, and the pain is greatly reduced,” Shissler adds. “I actually have days where there is no pain.”