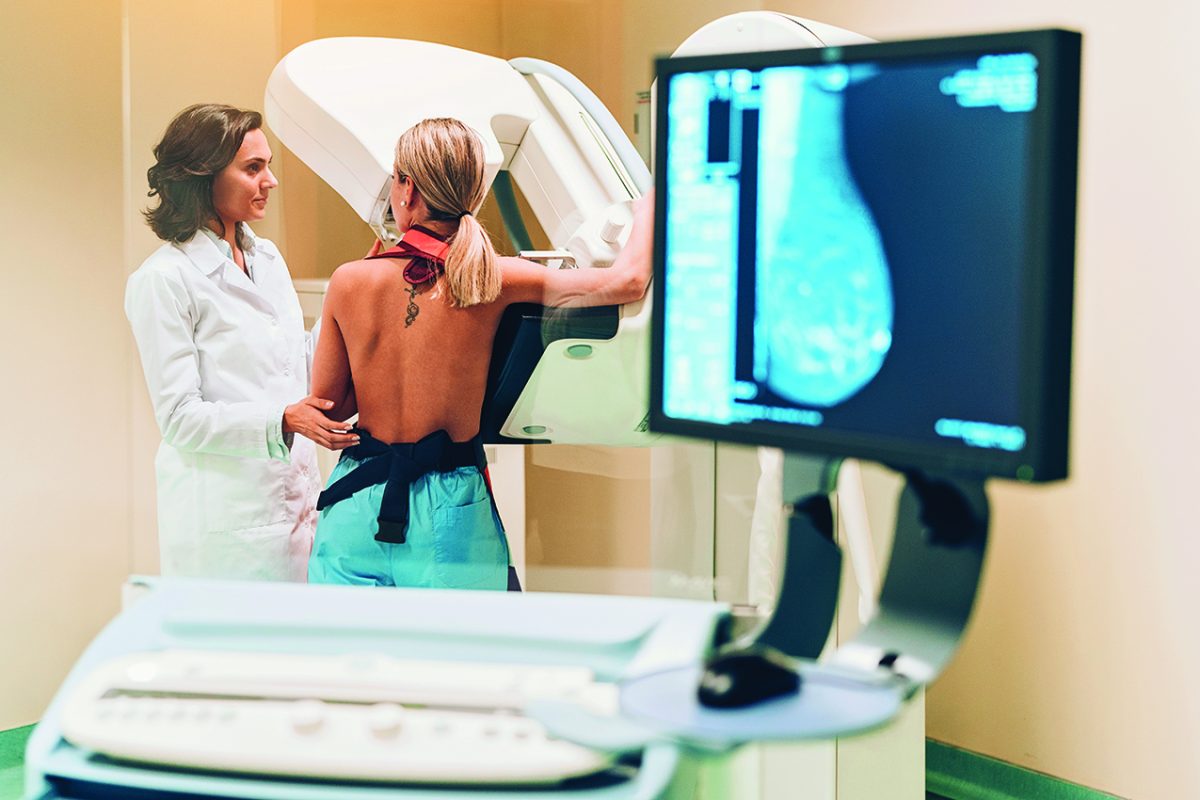
Breast cancer: More warning signs than just a lump
Do you know the warnings signs of breast cancer?
It’s the most common cancer in women in the United States, except for skin cancers, yet a new national survey finds many adults don’t know what to look for beyond a telltale lump. A survey by The Ohio State University Comprehensive Cancer Center found that while 9 out of 10 adults identify a lump in the breast as a symptom of breast cancer, far fewer know about other common symptoms that could also be associated with the disease. Medical experts say those results are concerning because many breast cancers do not present with a lump that can be detected by touch.
“The most frequent symptom that leads to a breast cancer diagnosis is a palpable lump,” says Dr. Matthew Miller, Breast Imaging Radiologist with the Allegheny Health Network (AHN) Imaging Institute. “However, most lumps are not cancer and there are other symptoms that can lead to a breast cancer diagnosis as well.”
Less Common Symptoms
Miller says breast pain might be the most commonly evaluated symptom in the breast center and that it rarely leads to a cancer diagnosis.
“All pain should be evaluated,” he cautions, “but when the pain is constant and focal, the concern is slightly increased … but it’s still low.”
When it comes to breast cancer, other symptoms may be less common but are often more concerning including:
n Nipple changes such as retraction, inversion, or a change in color.
n Skin changes such as dimpling, worsening redness, or ulceration
n Nipple discharge especially unilateral, clear, or bloody.
n Pitting/thickening of the skin on the breast.
The survey results showing a lack of awareness of these symptoms highlights why staying up to date on breast cancer screenings is so important. However, when it comes to recommendations for screenings, many women say they’re not even sure where the current medical guidance stands.
One-third of women in the OSU survey said they are confused about recommendations for breast cancer screenings, particularly those under age 30. That frustration is also shared by many medical professionals.
“I can tell you that providers are definitely frustrated,” stresses Miller. “When the U.S. Preventive Services Task Force (USPSTF) came out with divergent recommendations a number of years ago, it definitely led to an increase in confusion among providers and patients alike. The good news is that providers, advocates, and interest groups do a fantastic job at spreading awareness of the fact that annual mammography starting at age 40 (or earlier for high-risk patients) saves the most lives. If everyone recognizes and acknowledges this important fact, then the recommendation becomes clear.”
Those recommendations currently advise average risk women should start getting 3D mammograms every year starting at the age of 40. This gives breast imagers the best chance to detect a developing cancer early enough to easily treat it and gives patients the best chance of surviving a screen-detected cancer.
For high-risk patients, the recommendation is different.
“Genetic mutations, family history, and prior radiation exposure can affect your lifetime risk for developing breast cancer,” explains Miller. “We recommend having that risk conversation with your primary care provider at the age of 30 or earlier if you have a suspicion. If you’re deemed a ‘high risk’ patient, you will likely need to start screening mammography earlier, and will also likely qualify for a screening breast MRI. Bottom line, talk to your doctor who will guide you.”
Besides doing mammograms and self-exams, doctors encourage women to develop a baseline understanding of what their breasts look and feel like and be comfortable recognizing any changes.
“Hormone fluctuations can induce changes in your breast, so symptoms that come and go and are usually not cause for concern,” says Miller. “But if you notice a change that persists for a few weeks or more, you should make an appointment to be seen at a breast center. Chances are that the evaluation will be normal; however, it’s better to be safe than sorry.”
He also stresses this advice goes for men, too. While there are no current screening guidelines for men regarding breast cancer, 1% of breast cancer occurs in men.
“It’s important for men to recognize any changes in their breasts and promptly get evaluated when necessary,” Miller adds. “The most important thing a patient can do to give themselves the best chance at surviving a breast cancer diagnosis is to get their mammogram every year and never ignore a symptom. If you adhere to these two recommendations, the chances are quite good that breast cancer, if it happens, will just be a bump in the road of your life.”